How To Remove Bunions Without Surgery
Overview
![]() Bunions are a common problem that most individuals experience as a painful swelling or a bony protuberance at the inner base of the big toe. This condition is the result of a malalignment of the first toe. These can be hereditary or secondary to wearing high-heeled or narrow toe-box shoes.
Bunions are a common problem that most individuals experience as a painful swelling or a bony protuberance at the inner base of the big toe. This condition is the result of a malalignment of the first toe. These can be hereditary or secondary to wearing high-heeled or narrow toe-box shoes.
Causes
Inflammatory joint diseases. Those who suffer from rheumatoid and psoriatic arthritis are at risk for bunions, although many times, those who suffer from bunions will mistakenly attribute the soreness in their feet to arthritis. Genetic and neuromuscular factors. Individuals with Down?s Syndrome are believed to be more prone to developing bunions; therefore, the gait and feet of such patients should be examined carefully and regularly so that any problems can be caught and treated early. Similarly, individuals of any age who have been diagnosed with Ehlers-Danlos or Marfan?s Syndrome, have also been shown to have a higher than average occurrence of bunions. Limb inequality. Individuals who have legs of unequal length often suffer from bunions on the longer limb due to the irregular mechanics of their walking or running gait.
Symptoms
With Bunions, a person will have inflammation, swelling, and soreness on the side surface of the big toe. Corns most commonly are tender cone-shaped patches of dry skin on the top or side of the toes. Calluses will appear on high-pressure points of the foot as thick hardened patches of skin.
Diagnosis
Your family doctor or chiropodist /podiatrist can identify a bunion simply by examining your foot. During the exam, your big toe will be moved up and down to determine if your range of motion is limited. You will be examined for signs of redness or swelling and be questioned about your history of pain. A foot x-ray can show an abnormal angle between the big toe and the foot. In some cases, arthritis may also be seen. A X-ray of your foot may help identify the cause of the bunion and rate its severity.
Non Surgical Treatment
If you suspect a bunion, it is essential that you confirm your suspicions by consulting with a podiatric physician. Don?t try to treat the problem yourself, even by using conservative measures. Many conditions have similar symptoms, and only a professional can tell the difference. Once a diagnosis is obtained, it is essential to begin treatment immediately. Your podiatric physician will advise you on the most effective means. If caught early enough, good foot care, shoes that fit properly, and/or orthoses may eliminate the need for any further intervention. Certain over-the-counter remedies, such as felt or foam pads, applied to specific areas of the foot to relieve pressure and friction, will protect the bunion. Elevating the foot and icing the area for 20 minutes an hour may help to relieve pain. 
Surgical Treatment
Bunion surgery is most often done on an outpatient or day-surgery basis, usually with a local anesthetic technique called an ankle block. The surgery typically takes an hour or two to perform. Following your surgery, you will stay in the Recovery Room for several hours while the anesthetic wears off. For your safety, you will be required to have someone to drive you home. You should keep in mind that any surgery carries with it very small-but-possible risks of complications such as allergic reaction to anesthesia, bleeding and infection.
What Is Overpronation Of The Feet
Overpronation can affect people of all ages and it is particularly problematic for patients with high levels of activity. This problem is generally present at birth. Overpronation occurs with EVERY STEP taken. Considering the average person takes almost 8,000 steps per day and millions of steps in a lifetime, it's easy to see how the cumulative trauma from the unbalanced strain and excessive forces can lead to serious damage.

Causes
Flat feet don't automatically mean you have a problem. The problem can be divided into a flexible flat foot or rigid flat foot. The rigid flat foot is one that does not change shape when the foot becomes weight bearing. i.e. it does not go through the excessive motion of pronation. Generally speaking this foot does not provide too many problems. The flexible flat foot is the type that when it becomes weight bearing the foot and ankle tends to roll in (pronates) too far. This type of person will often say I have great arches but when I stand up much of this arch disappears as the foot excessively pronates When the foot is excessively pronating and causing problems like sore ankles, feet or knees when standing or exercising then arch support is extremely important to restore the foot structure.
Symptoms
It is important to note that pronation is not wrong or bad for you. In fact, our feet need to pronate and supinate to achieve proper gait. Pronation (rolling inwards) absorbs shock and supination (rolling outwards) propels our feet forward. It is our body?s natural shock-absorbing mechanism. The problem is over-pronation i.e. the pronation movement goes too deep and lasts for too long, which hinders the foot from recovering and supinating. With every step, excess pronation impedes your natural walking pattern, causing an imbalance in the body and consequent excessive wear and tear in joints, muscles and ligaments. Some common complaints associated with over-pronation include Heel Pain (Plantar Fasciitis) ,Ball of foot pain, Achilles Tendonitis, Shin splints, Knee Pain, Lower Back Pain.
Diagnosis
Pronounced wear on the instep side of shoe heels can indicate overpronation, however it's best to get an accurate assessment. Footbalance retailers offer a free foot analysis to check for overpronation and help you learn more about your feet.

Non Surgical Treatment
The way a foot orthotic works is by altering the weight-bearing surface of the foot. The simulated foot improvement is only possible when standing still with full weight applied. Orthotics are of little help through most of the actual walking cycle. observationPatients may experience some symptom relief, but the orthotic cannot correct the internal osseous misalignment. Over-the-counter foot orthotics are usually of little help and wear out quickly. Custom-made foot orthotics, obtained through your doctor's office, are generally expensive. Though they last longer and have less chance of ill-effects than OTC brands, they still need to be replaced often. Over a lifetime, an individual can spend several thousands of dollars in total costs associated with orthotics and see little or no results. This is because orthotics only work when you are wearing them and do not treat the cause of the problem. In many cases, the external pressure points created by orthotics can cause more problems than solutions. Blisters, sore feet, sore joints and many other long-term complications can arise as a consequence of wearing orthotics.
Surgical Treatment
Depending on the severity of your condition, your surgeon may recommend one or more treatment options. Ultimately, however, it's YOUR decision as to which makes the most sense to you. There are many resources available online and elsewhere for you to research the various options and make an informed decision.
Calcaneal Apophysitis In Youngsters
Sever's disease, or calcaneal apophysitis, is a common cause of heel pain in patients whose bones are still growing; however, it is not really a disease. The pain is caused by stress at the point where the Achilles tendon meets tissue called the plantar fascia on the growth plate (apophysis) of the heel bone (calcaneus). Sever's affects boys more often than girls. Boys are most often affected at age 12, and girls at age 9, though Sever's is typically seen in children and adolescents between the ages of 7 and 15.
Causes
Sever?s disease is often associated with a growth spurt, when the bones grow but the muscles do not. Therefore the muscles effectively become tighter which results in increased stress at the heel. It may also be related to unusual biomechanics, for instance poor foot posture, muscle tightness or muscle weakness. Overtraining or incorrect training can also play a part. Usually, the cause is a combination of factors.
Symptoms
Patients with Severs disease typically experience pain that develops gradually in the back of the heel or Achilles region. In less severe cases, patients may only experience an ache or stiffness in the heel that increases with rest (especially at night or first thing in the morning). This typically occurs following activities which require strong or repetitive contraction of the calf muscles, such as running (especially uphill) or during sports involving running, jumping or hopping. The pain associated with this condition may also warm up with activity in the initial stages of the condition. As the condition progresses, patients may experience symptoms that increase during activity and affect performance. Pain may also increase when performing a calf stretch or heel raise (i.e. rising up onto tip toes). In severe cases, patients may walk with a limp, have difficulty putting their heel down, or be unable to weight bear on the affected leg. Pain may also increase on firmly touching the affected region and occasionally a bony lump may be palpable or visible at the back of the heel. This condition typically presents gradually overtime and can affect either one or both lower limbs.
Diagnosis
Sever?s disease is diagnosed based on a doctor?s physical examination of the lower leg, ankle, and foot. If the diagnosis is in question, the doctor may order x-rays or an MRI to determine if there are other injuries that may be causing the heel pain.
Non Surgical Treatment
The disease itself is self limiting and will resolve regardless of treatment once the growth plate has fully closed. Depending on the age of the youth at onset this could be a problem for many years. Treatment has always been aimed at managing the pain as well as the inflammation. This is done with the rest, ice, non steroidal anti-inflammatories like ibuprofen, stretching, taping, heel cups, heel lifts and orthotics. In severe cases, cast or walking boot immobilization is used. Each of these have differing levels of efficacy but in my experience orthotics are the golden treatment or the silver bullet. I am not talking about your run of the mill over the counter Dr. Scholls shoe insert. These definitely have their place in the world but not here. Custom molded orthotics made from a mold taken of the youths foot will provide the necessary control and support to stop the pain cycle. We can safely report over 85% of patients who are able to get back to sports and other activities as long as they wear the orthotics in supportive shoes as directed.
Prevention
To reduce the risk of heel pain or sore heels from Sever?s Disease. Only wear properly fitting shoes. A lace up shoe with a firm heel counter. Stretch calf and foot before exercising or playing sports. Properly taping the foot provides excellent protection and immediate pain relief. Wear shoe inserts or an over-the-counter orthotic. If the problem persists, consult your foot doctor.
Posterior Tibial Tendon Dysfunction (PTTD) Treatment And Cause
Overview
Posterior tibial tendon insufficiency (also called posterior tibial tendon dysfunction or adult acquired flatfoot) has been named literally after failure of the posterior tibial tendon. However, the condition is caused not only by the progressive failure of the posterior tibial tendon; it is also failure of associated ligaments and joints on the inner side of the ankle and foot. This results in collapse of the arch of the foot, along with the deformity which most often becomes the debilitating problem in its later stages. While at the beginning the common symptom is pain over the tendon in the inner part of the hindfoot and midfoot, later on it is the deformity that can threaten a person?s ability to walk. Just as the tendon degenerates and loses its function, other soft tissue on the same inner side of the foot - namely the ligaments - degenerate and fail. Ligaments are responsible for holding bones in place, and when they fail, bones shift to places where they shouldn?t; deformity is the result. The deformity causes malalignment, leading to more stress and failure of the ligaments. 
Causes
As discussed above, many different problems can create a painful flatfoot. Damage to the posterior tibial tendon is the most common cause of AAFD. The posterior tibial tendon is one of the most important tendons of the leg. It starts at a muscle in the calf, travels down the inside of the lower leg and attaches to the bones on the inside of the foot. The main function of this tendon is to support the arch of your foot when you walk. If the tendon becomes inflamed or torn, the arch will slowly collapse. Women and people over 40 are more likely to develop problems with the posterior tibial tendon. Other risk factors include obesity, diabetes, and hypertension. Having flat feet since childhood increases the risk of developing a tear in the posterior tibial tendon. In addition, people who are involved in high impact sports, such as basketball, tennis, or soccer, may have tears of the tendon from repetitive use. Inflammatory arthritis, such as rheumatoid arthritis, can cause a painful flatfoot. This type of arthritis attacks not only the cartilage in the joints, but also the ligaments that support the foot. Inflammatory arthritis not only causes pain, but also causes the foot to change shape and become flat. The arthritis can affect the back of the foot or the middle of foot, both of which can result in a fallen arch. An injury to the tendons or ligaments in the foot can cause the joints to fall out of alignment. The ligaments support the bones and prevent them from moving. If the ligaments are torn, the foot will become flat and painful. This more commonly occurs in the middle of the foot (Lisfranc injury), but can also occur in the back of the foot. Injuries to tendons of the foot can occur either in one instance (traumatically) or with repeated use over time (overuse injury). Regardless of the cause, if tendon function is altered, the forces that are transmitted across joints in the foot are changed and this can lead to increased stress on joint cartilage and ligaments. In addition to tendon and ligament injuries, fractures and dislocations of the bones in the midfoot can also lead to a flatfoot deformity. People with diabetes or with nerve problems that limits normal feeling in the feet, can have collapse of the arch or of the entire foot. This type of arch collapse is typically more severe than that seen in patients with normal feeling in their feet. In addition to the ligaments not holding the bones in place, the bones themselves can sometimes fracture and disintegrate without the patient feeling any pain. This may result in a severely deformed foot that is very challenging to correct with surgery. Special shoes or braces are the best method for dealing with this problem.
Symptoms
In many cases, adult flatfoot causes no pain or problems. In others, pain may be severe. Many people experience aching pain in the heel and arch and swelling along the inner side of the foot.
Diagnosis
The diagnosis of posterior tibial tendon dysfunction and AAFD is usually made from a combination of symptoms, physical exam and x-ray imaging. The location of pain, shape of the foot, flexibility of the hindfoot joints and gait all may help your physician make the diagnosis and also assess how advanced the problem is.
Non surgical Treatment
Although AAF is not reversible without surgery, appropriate treatment should address the patient?s current symptoms, attempt to reduce pain, and allow continued ambulation. In the early stages, orthotic and pedorthic solutions can address the loss of integrity of the foot?s support structures, potentially inhibiting further destruction.3-5 As a general principle, orthotic devices should only block or limit painful or destructive motion without reducing or restricting normal motion or muscle function. Consequently, the treatment must match the stage of the deformity. 
Surgical Treatment
Until recently, operative treatment was indicated for most patients with stage 2 deformities. However, with the use of potentially effective nonoperative management , operative treatment is now indicated for those patients that have failed nonoperative management. The principles of operative treatment of stage 2 deformities include transferring another tendon to help serve the role of the dysfunctional posterior tibial tendon (usually the flexor hallucis longus is transferred). Restoring the shape and alignment of the foot. This moves the weight bearing axis back to the center of the ankle. Changing the shape of the foot can be achieved by one or more of the following procedures. Cutting the heel bone and shifting it to the inside (Medializing calcaneal osteotomy). Lateral column lengthening restores the arch and overall alignment of the foot. Medial column stabilization. This stiffens the ray of the big toe to better support the arch. Lengthening of the Achilles tendon or Gastrocnemius. This will allow the ankle to move adequately once the alignment of the foot is corrected. Stage 3 acquired adult flatfoot deformity is treated operatively with a hindfoot fusion (arthrodesis). This is done with either a double or triple arthrodesis - fusion of two or three of the joints in hindfoot through which the deformity occurs. It is important when a hindfoot arthrodesis is performed that it be done in such a way that the underlying foot deformity is corrected first. Simply fusing the hindfoot joints in place is no longer acceptable.
Adult Aquired FlatFoot
PTTD is a common condition treated by foot and ankle specialists. Although there is a role for surgical treatment of PTTD, conservative care often can prevent or delay surgical intervention. Decreasing inflammation and stabilizing the affected joints associated with the posterior tibial tendon can decrease pain and increase functional levels. With many different modalities available, aggressive nonoperative methods should be considered in the treatment of PTTD, including early immobilization, the use of long-term bracing, physical therapy, and anti-inflammatory medications. If these methods fail, proper evaluation and work-up for surgical intervention should be employed.
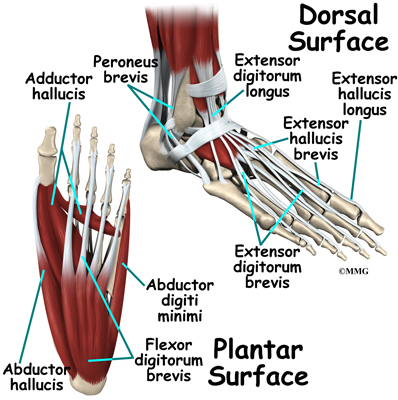
Causes
Several risk factors are associated with PTT dysfunction, including high blood pressure, obesity, diabetes, previous ankle surgery or trauma and exposure to steroids. A person who suspects that they are suffering from PTT dysfunction should seek medical attention earlier rather than later. It is much easier to treat early and avoid a collapsed arch than it is to repair one. When the pain first happens and there is no significant flatfoot deformity, initial treatments include rest, oral anti-inflammatory medications and, depending on the severity, a special boot or brace.
Symptoms
Pain and swelling behind the inside of your ankle and along your instep. You may be tender behind the inner ankle where the posterior tibial tendon courses and occasionally get burning, shooting, tingling or stabbing pain as a result of inflammation of the nerve inside the tarsal tunnel. Difficulty walking, the inability to walk long distances and a generalised ache while walking even short distances. This may probably become more pronounced at the end of each day. Change in foot shape, sometimes your tendon stretches out, this is due to weakening of the tendon and ligaments. When this occurs, the arch in your foot flattens and a flatfoot deformity occurs, presenting a change in foot shape. Inability to tip-toe, a way of diagnosing Posterior Tibial Tendon Dysfunction is difficulty or inability to ?heel rise? (stand on your toes on one foot). Your tibialis posterior tendon enables you to perform this manoeuvre effectively. You may also experience pain upon attempting to perform a heel rise.
Diagnosis
In diagnosing flatfoot, the foot & Ankle surgeon examines the foot and observes how it looks when you stand and sit. Weight bearing x-rays are used to determine the severity of the disorder. Advanced imaging, such as magnetic resonance imaging (MRI) and computed tomography (CAT or CT) scans may be used to assess different ligaments, tendons and joint/cartilage damage. The foot & Ankle Institute has three extremity MRI?s on site at our Des Plaines, Highland Park, and Lincoln Park locations. These extremity MRI?s only take about 30 minutes for the study and only requires the patient put their foot into a painless machine avoiding the uncomfortable Claustrophobia that some MRI devices create.
Non surgical Treatment
Treatment of Adult Acquired Flatfoot Deformity depends on the stage of progression, as mentioned above paragraphs. Below we will outline a variety of different treatment options available. Orthotics or bracing. To give your foot the arch the support it needs, your podiatrist or foot specialist may provide you with over the counter brace or a custom orthotic device that fits your shoe. Casting. In some cases, a cast or boot is worn to stabilize the foot and to give the tendon time to heal. Physiotherapy. Ultrasound treatments and exercises may help rehab the tendon and muscles. Medications. Over-the-counter (NSAIDS) such as ibuprofen can help reduce pain, inflammation and swelling associated with AAFD. Shoe Gear. Your podiatrist may suggest changes with your shoes you are wearing and inserts you need in your shoe to help support your arch.
Surgical Treatment
If cast immobilization fails, surgery is the next alternative. Treatment goals include eliminating pain, halting deformity progression and improving mobility. Subtalar Arthroereisis, 15 minute outpatient procedure, may correct flexible flatfoot deformity (hyperpronation). The procedure involves placing an implant under the ankle joint (sinus tarsi) to prevent abnormal motion. Very little recovery time is required and it is completely reversible if necessary. Ask your Dallas foot doctor for more information about this exciting treatment possibility.
What Are The Key Treatment And Cause Of Achilles Tendonitis ?
 Typically an overuse injury, Achilles tendinitis affects the connective tissue between the calf and the heel. When you walk, run or otherwise use your leg to push your body upward, the Achilles tendon is engaged. Using the tendon frequently and with high intensity often results in tendinitis -- a swollen Achilles tendon that makes it difficult and sometimes painful to continue high-impact activities.
Typically an overuse injury, Achilles tendinitis affects the connective tissue between the calf and the heel. When you walk, run or otherwise use your leg to push your body upward, the Achilles tendon is engaged. Using the tendon frequently and with high intensity often results in tendinitis -- a swollen Achilles tendon that makes it difficult and sometimes painful to continue high-impact activities.
Causes
Achilles tendonitis is an overuse injury. Too much too soon is the common cause of overuse injuries, however other factors can contribute to developing the condition. An increase in activity, either distance, speed or a sudden change to running up hills. As a rule of thumb distance runners should increase their mileage by no more than 10% per week. A change of footwear or training surface for example suddenly running on soft sand can cause the heel to drop lower than normal making the tendon stretch further than it is used to. Weak calf muscles can tighten or go into partial spasm which again increases the strain on the achilles tendon by shortening the muscle. Running up hills - the achilles tendon has to stretch more than normal on every stride. This is fine for a while but will mean the tendon will fatigue sooner than normal. Overpronation or feet which roll in when running can place an increased strain on the achilles tendon. As the foot rolls in (flattens) the lower leg also rotates inwards which places twisting stresses on the tendon. Wearing high heels constantly shortens the tendon and calf muscles. When exercising in flat running shoes, the tendon is stretched beyond its normal range which places an abnormal strain on the tendon.
Symptoms
Achilles tendonitis may be felt as a burning pain at the beginning of activity, which gets less during activity and then worsens following activity. The tendon may feel stiff first thing in the morning or at the beginning of exercise. Achilles tendonitis usually causes pain, stiffness, and loss of strength in the affected area. The pain may get worse when you use your Achilles tendon. You may have more pain and stiffness during the night or when you get up in the morning. The area may be tender, red, warm, or swollen if there is inflammation. You may notice a crunchy sound or feeling when you use the tendon.
Diagnosis
Examination of the achilles tendon is inspection for muscle atrophy, swelling, asymmetry, joint effusions and erythema. Atrophy is an important clue to the duration of the tendinopathy and it is often present with chronic conditions. Swelling, asymmetry and erythema in pathologic tendons are often observed in the examination. Joint effusions are uncommon with tendinopathy and suggest the possibility of intra-articular pathology. Range of motion testing, strength and flexibility are often limited on the side of the tendinopathy. Palpation tends to elicit well-localized tenderness that is similar in quality and location to the pain experienced during activity. Physical examinations of the Achilles tendon often reveals palpable nodules and thickening. Anatomic deformities, such as forefoot and heel varus and excessive pes planus or foot pronation, should receive special attention. These anatomic deformities are often associated with this problem. In case extra research is wanted, an echography is the first choice of examination when there is a suspicion of tendinosis. Imaging studies are not necessary to diagnose achilles tendonitis, but may be useful with differential diagnosis. Ultrasound is the imaging modality of first choice as it provides a clear indication of tendon width, changes of water content within the tendon and collagen integrity, as well as bursal swelling. MRI may be indicated if diagnosis is unclear or symptoms are atypical. MRI may show increased signal within the Achilles.
Nonsurgical Treatment
Nonsurgical methods include rest and stop doing activities that cause stress to the tendon. Ice the area by applying ice to the tendon for 15 minutes after exercising. Compress the tendon by using an athletic wrap or surgical tape. Elevate your injury. You can reduce swelling by lying down and raising your foot at a level that is above your heart. Stretch your ankles and calf muscles. Take anti-inflammatory medication (e.g.: ibuprofen to reduce swelling). Wear orthotics and running shoes. Take part in physical therapy.

Surgical Treatment
It is important to understand that surgery may not give you 100% functionality of your leg, but you should be able to return to most if not all of your pre-injury activities. These surgical procedures are often performed with very successful results. What truly makes a difference is your commitment to a doctor recommended rehabilitation program after surgery as there is always a possibility of re-injuring your tendon even after a surgical procedure. One complication of surgical repair for Achilles tendon tear is that skin can become thin at site of incision, and may have limited blood flow.
Prevention
The following measures can significantly reduce the risk of developing Achilles tendonitis. Adequately stretch and warm up prior to exercise. Warm down and stretch after exercise. Choose footwear carefully and use footwear appropriate to the sport being undertaken. Use orthotic devices in footwear to correctly support the foot. Exercise within fitness levels and follow a sensible exercise programme. Develop strong, flexible calf muscles.
What Is Plantar Fasciitis And Methods To Get Rid Of It
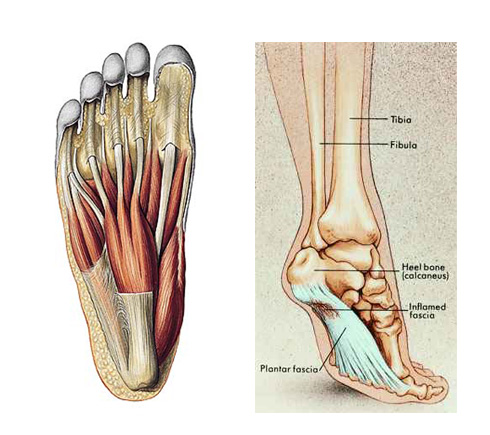
Overview
Plantar fasciitis is sometimes mixed up with a heel spur although they are not the same. A heel spur is a calcium deposit that occurs where the plantar fascia is attached to the heel bone (calcaneus). In many cases a heel spur is found on a foot with no pain or other symptoms at all. And in many painful heels there is no sign for a heel spur. Heel spur and painful heal does not necessarily go together. For many years plantar fasciitis was believed to be an inflammatory condition. It is thought now to be inaccurate because there were many cases of the disorder with no inflammatory signs observed within the fascia. The heel pain cause is now believed to be damage to the collagen fibers of the fascia. This damage, caused by stress injury, sometimes may include inflammatory cells.
Causes
When the foot moves, the plantar fascia stretches and contracts. Plantar fasciitis is caused by the repetitive overstretching of the plantar fascia. If the tension on the plantar fascia is too great, this overstretching causes small tears in the plantar fascia. This in turn causes the plantar fascia to become inflamed and painful. Factors that contribute to the development of plantar fasciitis include having very high arches or flat feet, gender, while anyone can develop plantar fasciitis, it tends to occur more commonly in women, exercises such as running, walking and dancing, particularly if the calf muscles are tight. Activities or occupations that involve walking or standing for long periods of time, particularly on hard surfaces, wearing high heeled shoes or shoes that do not offer adequate arch support and cushioning, being overweight, additional weight increases the tension on the plantar fascia, poor biomechanics, extra tension is placed on the plantar fascia if weight is not spread evenly when standing, walking or running. Some cases of plantar fasciitis may be linked to underlying diseases that cause arthritis, such as ankylosing spondylitis.
Symptoms
The most obvious symptom of plantar fasciitis is a sharp pain on the bottom of the foot, near the heel. Here are some signals that this pain may be plantar fasciitis. The pain is strongest first thing in the morning but gets better after a few minutes of walking around. The pain is worse after standing for a long time or after getting up from sitting. The pain develops gradually and becomes worse over time. The pain is worse after exercise or activity than it is during activity. It hurts when stretching the foot. It hurts when pressing on the sides of the heel or arch of the foot.
Diagnosis
The health care provider will perform a physical exam. This may show tenderness on the bottom of your foot, flat feet or high arches, mild foot swelling or redness, stiffness or tightness of the arch in the bottom of your foot. X-rays may be taken to rule out other problems.
Non Surgical Treatment
In the early stages of plantar fasciitis resting the foot may ease the pain. Medication to reduce inflammation should help but should only be used short term. Strapping may temporarily reduce the pain. All of the above therapies are only temporary measures and the pain is likely to reoccur if the cause of the abnormal pressure which has triggered the plantar fasciitis has not been identified. In order to establish the cause of the plantar fasciitis a biomechanical assessment may be required.

Surgical Treatment
Surgery for plantar fasciitis can be very successful in the right patients. While there are potential complications, about 70-80% of patients will find relief after plantar fascia release surgery. This may not be perfect, but if plantar fasciitis has been slowing you down for a year or more, it may well be worth these potential risks of surgery. New surgical techniques allow surgery to release the plantar fascia to be performed through small incisions using a tiny camera to locate and cut the plantar fascia. This procedure is called an endoscopic plantar fascia release. Some surgeons are concerned that the endoscopic plantar fascia release procedure increases the risk of damage to the small nerves of the foot. While there is no definitive answer that this endoscopic plantar fascia release is better or worse than a traditional plantar fascia release, most surgeons still prefer the traditional approach.